 Health & Physiology
Health & Physiology
Powering up the emergency response to infections
All blood cells are made in the bone marrow with an estimated production of 1 million white cells per second. In response to infection white cell production increases threefold. Such a production requires energy provided by mitochondria. Our study reveals how blood stem cells acquire mitochondria from support cells, without which our immune system would not function.
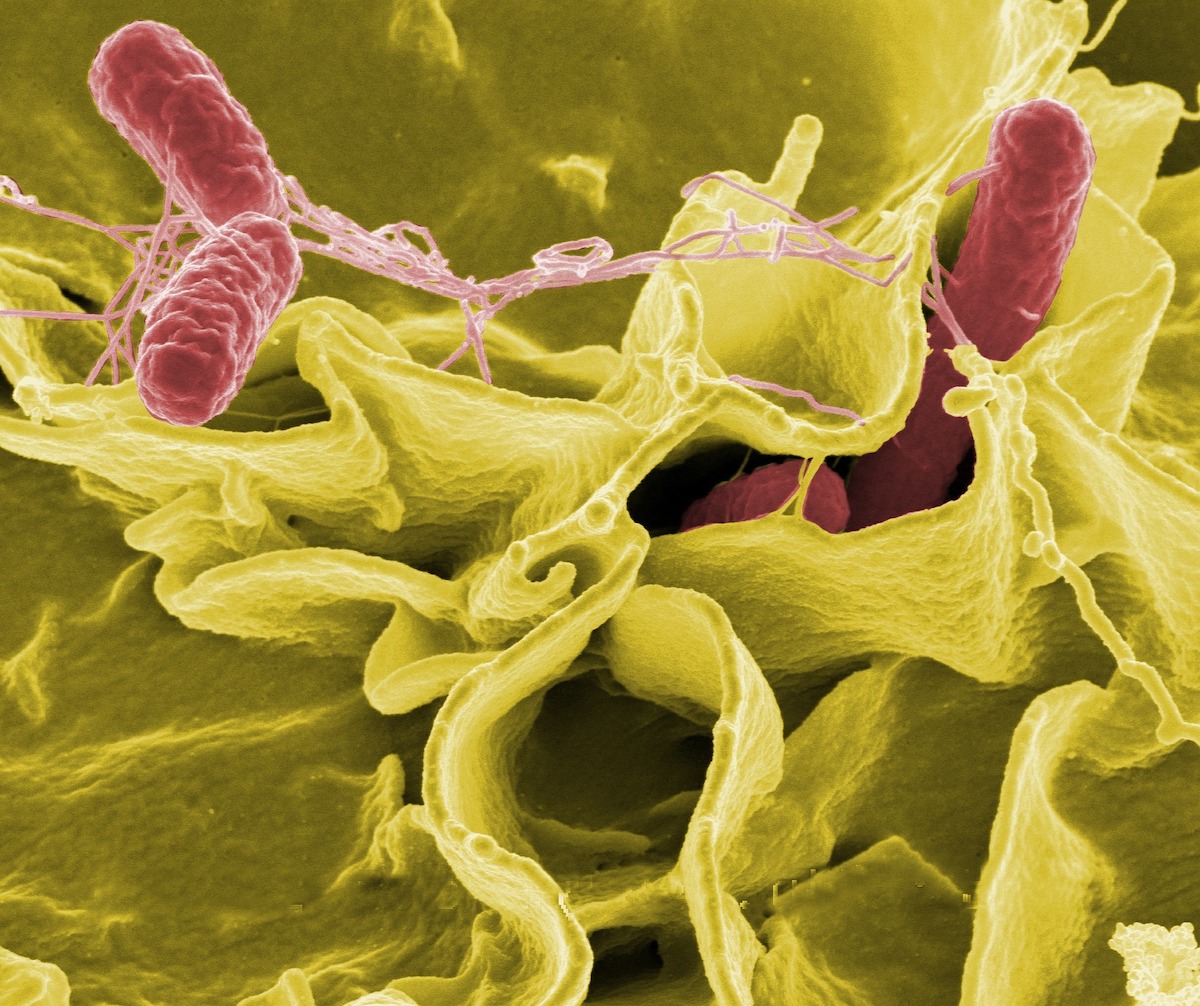
Salmonella is a bacterial infection and one of the most common causes of food poisoning worldwide. Symptoms can include diarrhoea, vomiting, abdominal pain and fever. The majority of people recover within a few days without treatment, however, people who have a weakened immune system including young children and the elderly are at a greater risk of becoming critically ill.
The immune system is made up of many cell types which develop from immature cells called blood stem cells. This process, better known as haematopoiesis, occurs in the bone marrow and requires the support of non-blood cells.
An average human produces around one trillion mature blood cells per day. This number increases during infections such as Salmonella. Increased haematopoiesis requires a lot of energy, but it is still unclear how blood stem cells acquire enough energy to respond to such challenges. In our study we found that the stem cells rely on other cells to provide the energy needed for the immune system response.
Cells make their energy in structures called mitochondria, which are like tiny batteries providing the energy in the form of a molecule called ATP. ATP is produced in the mitochondria from sugar and fat with the help of oxygen, a process known as oxidative phosphorylation (OXPHOS). The mitochondria move around the cell in networks and are constantly fusing and splitting from this network to provide ATP to the parts of the cell that need it.
In response to Salmonella infection blood stem cells can acquire more energy by increasing the amount of mitochondria within 2 hours of sensing the infection. How is this possible? To determine if more mitochondria are supplied to the blood stem cells by bone marrow support cells, we generated a humanized mouse model. This model has human blood stem cells, but all bone marrow support cells come from the mouse. This enables us to determine if mitochondria are transferred from mouse cells to human cells, as we can easily recognize the mouse mitochondria inside the human cells. To simulate infection, we exposed these humanized animals to Salmonella components and discovered that the isolated blood stems cells contained mouse mitochondria. Together with other experiments, this confirmed that mitochondria could move from bone marrow support cells to blood stem cells in response to infection.
We then wanted to know if the transferred mitochondria allowed the blood stem cells to produce more ATP, which would allow increased blood cell production. We showed that blood stem cells from Salmonella infected animals had increased OXPHOS and consequently more ATP. Moreover, we found out that blocking ATP production prevented mitochondrial transfer from support cells to blood stem cells.
Finally, we wanted to determine which support cells of the bone marrow were donating their mitochondria to blood stem cells. We examined a number of different types of cells found in the bone marrow and discovered that the stromal cells are responsible for this transfer of mitochondria. Moreover, we discovered that direct cell-to-cell contact was required between them for this transfer of mitochondria to occur.
In conclusion, we found that the stromal cells of bone marrow transfer their power-generating mitochondria to neighbouring blood stem cells to enhance generation of immune cells, which are required for our body's response to infections. We showed that stromal cells and blood stem cells have to come in direct contact for mitochondrial transfer to occur and that if mitochondrial transfer is blocked, the infection is not fought. Our discoveries strengthen our knowledge on the body's fight against infections and we hope they will contribute to the development of new therapeutic approaches in the future.
Original Article:
Mistry J, Marlein C, Moore J et al. ROS-mediated PI3K activation drives mitochondrial transfer from stromal cells to hematopoietic stem cells in response to infection. Proceedings of the National Academy of Sciences. 2019;116(49):24610-24619.Next read: Mitochondria as microlenses in the eye – the evolution of an improved camera sensor by John M. Ball , Wei Li
Edited by:
Dr. Giacomo Rossetti , Senior Scientific Editor
We thought you might like
Living without mitochondria: the downfall of one textbook truth
Oct 3, 2016 in Evolution & Behaviour | 3.5 min read by Lukáš NovákExercise helps restore aged muscles
Apr 20, 2018 in Health & Physiology | 3.5 min read by Matthew Robinson , Sreekumaran NairThe mystery of mistletoe mitochondria
Dec 21, 2018 in Evolution & Behaviour | 4 min read by Andrew Maclean , Janneke Balk , Etienne MeyerMore than meets the eye: the histones revealed as enzymes
Jan 12, 2021 in Health & Physiology | 3 min read by Oscar A. Campos , Siavash K. KurdistaniMore from Health & Physiology
Tobacco smoking and other exposures shut off cancer-fighting genes
Aug 31, 2024 in Health & Physiology | 3 min read by Jüri Reimand , Nina AdlerA hidden clock that times cytoplasmic divisions
Aug 30, 2024 in Health & Physiology | 3 min read by Cindy OwWhen two kinases go for a dance
Aug 2, 2024 in Health & Physiology | 4 min read by Ioannis Galdadas , Francesco Luigi Gervasio , Pauline JuyouxAwakening the thymus to cure SARS-CoV-2 infection: a matter of genes
Jul 27, 2024 in Health & Physiology | 3.5 min read by Stefano Marullo , Cheynier RemiKeeping the balance: How epigenetics monitors cancer genes
May 13, 2024 in Health & Physiology | 4 min read by Zach Gray , Madison Honer , Johnathan WhetstineEditor's picks
Trending now
Popular topics


